Technology has made remarkable strides in cancer treatment, offering new hope and improved outcomes for patients worldwide. One of the most pivotal advancements in oncology is the development and use of linear accelerators (LINACs). These sophisticated machines are at the forefront of radiation therapy, providing targeted treatments to eradicate cancer cells while sparing healthy tissues.
What is a Linear Accelerator?
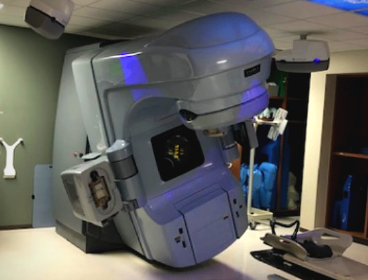
A linear accelerator (LINAC) is a device that uses high-energy X-rays or electrons to treat cancerous tumors. The technology is designed to deliver precise radiation therapy to cancerous tissues, which destroys the genetic material of cells, preventing them from growing and dividing. Linear accelerators are primarily used in external beam radiation therapy (EBRT), projecting high-energy beams directly into a tumor and minimizing the exposure to surrounding healthy tissue.
How Does a Linear Accelerator Work?
The operation of a linear accelerator involves several key components working seamlessly together:
Energy Generation: LINACs generate high-energy X-rays or electrons through a process called microwave technology. These high-energy beams are then accelerated to nearly the speed of light within the machine.
Shape and Focus: The beams are shaped and focused using a collimator that conforms the radiation beam to tumor’ shape. This shaping is crucial as it ensures the maximum dose is delivered to the cancer cells while minimizing damage to adjacent healthy tissue.
The Benefits of Using a Linear Accelerator in Cancer Treatment
Linear accelerators are beneficial for several reasons:
Precision and Flexibility: They provide a level of precision that significantly reduces the likelihood of damaging healthy tissues and organs adjacent to the tumor. This precision is particularly important for tumors located near critical structures like the spinal cord or brain.
Customizable for Individual Patients: Every cancer is unique, and so is every patient’s anatomy. LINACs can be programmed to deliver radiation in the dose and shape that perfectly matches the tumor’s size and form.
Versatility: LINACs can be used to treat cancer anywhere in the body, making them versatile tools in the fight against cancer. They are effective for a wide range of cancers, including prostate, breast, lung, and brain cancers.
Reduced Treatment Times: Treatments with linear accelerators are generally quick. Patients typically spend less time in treatment compared to traditional radiation therapy methods, which translates to more comfort and less stress for the patient.
Integration with Other Treatment Forms: Linear accelerators can be used in conjunction with other cancer treatment forms like chemotherapy and surgery, providing a comprehensive approach to cancer treatment that can be tailored to the needs of the individual patient.
The Impact of Linear Accelerators on Cancer Treatment
The introduction of linear accelerators has revolutionized cancer treatment, making radiation therapy quicker, safer, and more effective. By delivering high doses of radiation with exquisite accuracy, linear accelerators ensure that tumors get the maximum possible dose while healthy tissues are preserved, improving patient outcomes and reducing side effects.
Cancer treatment is a complex and evolving field, but linear accelerators represent a significant step forward in fighting this disease. As technology advances, LINACs’ capabilities continue to grow, allowing for even greater precision and effectiveness in cancer therapy. Their ability to deliver targeted radiation with high precision makes them an invaluable tool in the ongoing battle against cancer.
For OEM replacement parts of Linear Accelerators and Radiation Oncology equipment, contact RadParts today!
RadParts, a TTG Imaging Solutions Company, is the world’s largest independent distributor of OEM replacement parts. We specialize in low-cost parts for repairing linear accelerators and radiation equipment. Our mission is to provide high-quality, user-friendly, low-cost components and support for linear accelerators and radiation equipment. Contact RadParts at 877-704-3838 to learn more.
Written by the digital marketing team at Creative Programs & Systems: www.cpsmi.com